The red flush on your face that won’t go away? Those red acne-like bumps? They may not be due to your hormones, menopause or even acne—it may be rosacea.
Fast Facts
- It is a common disease affecting one in five to ten percent of people worldwide—statistics vary—and it often goes undiagnosed and untreated.
- Rosacea mostly affects people between 30 and 60 years of age.
- People who blush frequently are believed to face a higher level of risk, as are those who have had severe acne, acne cysts and nodules.
That persistent embarrassing red flush on your face may be due to a common and harmless medical condition called rosacea. It affects one in five to ten percent of people worldwide and often goes undiagnosed. Although harmless, Rosacea can affect self-esteem and confidence, and have a negative impact on people’s social and professional lives. Here’s all you need to know about rosacea and its treatments.
Rosacea is a chronic inflammatory skin condition affecting adults. It causes redness in the face, especially on the forehead, nose, cheeks and chin. In addition to the redness, some people with rosacea develop small pus-filled acne-like bumps or pustules and sore, dry and burning eyes, which can sometimes cause vision problems. Other symptoms of rosacea include a swollen nose and thickening of skin in affected areas.
It is a common disease affecting one in five to ten percent of people worldwide—statistics vary—and it often goes undiagnosed and untreated. Although often described as acne-like, rosacea is a different from acne. It is also sometimes mistaken for other skin problems, including eczema and allergies.
Usually rosacea appears in phases:
- At the pre-rosacea stage, people experience a tendency to blush and flush easily, which progresses to become a persistent redness, especially in the middle part of the face and nose. The redness is due to the dilation of blood vessels close to the surface of the skin.
- At the vascular phase, the skin becomes overly sensitive, and the small blood vessels on the cheeks and chin swell up visibly. Doctors refer to this as telangiectasia. Sometimes vascular rosacea occurs together with dandruff and oily skin.
- The next stage is referred to as inflammatory rosacea. Tiny red bumps appear on the already red areas of the face, spreading across the cheeks, nose, chin and forehead.
- Ocular rosacea affects the eyes, inflaming the inner eyelid skin, making it appear scaly and occurs in about half of those who experience rosacea.
- Late in the cycle, some rosacea sufferers, mostly middle-aged men, develop raised, round red bumps and a bulbous nose. This condition is called rhinophyma.
There is no known cure for rosacea, but, treatments can help control and minimise symptoms.
Who gets rosacea?
Rosacea mostly affects people between 30 and 60 years of age. However persistent flushing, the main sign of rosacea, can begin in the teenage years. Doctors believe that early diagnosis and treatment at this stage can prevent it from becoming worse later.
Rosacea affects both men and women, although women are more likely to develop the condition than men, especially when going through menopause. Men usually experience more severe symptoms.
People who blush frequently are believed to face a higher level of risk, as are those who have had severe acne, acne cysts and nodules.
Those with fair skin, light hair and blue eyes, such as those with Celtic or Scandinavian ancestry, are more vulnerable to rosacea than others. People with a family history of rosacea or severe acne are also more likely to get it than those without.
Causes
What exactly causes rosacea is not clearly understood. Researchers suspect that it may be due to a combination of genetic factors, vascular and inflammatory factors and environmental factors including chronic exposure to ultraviolet radiation.
Scientists trying to discover the causes of rosacea have found that
- Rosacea is at least partly a hereditary condition. Many people who develop it also have family members with rosacea.
- The immune system of the body is involved. It has been observed that people with acne-like rosacea tend to also have bacillus oleronius, a bacterium that causes their immune systems to overreact. Whether this is a cause of rosacea is not yet clear.
- A bug causing intestinal infection, H pylori, is common among people with rosacea and may also play a role. The connection is not definite proof. People who do not have rosacea can have H pylori infections.
- A mitecalled Demodex, an eight-legged relative of spiders that lives on everyone’s skin—in the oily pores of the nose, forehead and cheeks, and in the hair follicles of the eyebrows and eyelashes—could also be the reason for rosacea. Demodex mites eat facial oil or sebum and begin colonising the face at puberty. Although everyone has them—yes, eek, we know!—there is ten times more Demodex in the skin of people with rosacea than in people without. Researchers from the National University of Ireland believe they have found what causes rosacea: demodex feces. In case you are keen to learn more about it, here’s the link: Rosacea may be caused by mite faeces in your pores.
- Cathelicidin, a protein responsible for protecting the skin from inflection may also be responsible for the redness and swelling that occurs with rosacea.
Many things can make rosacea worse including alcohol, hot or spicy foods and beverages—including coffee and tea, exposure to sunlight and extreme temperatures, as in hot baths and saunas. Certain face creams, oils and topical steroids can aggravate rosacea. Anger, anxiety, stress and embarrassment also aggravate the condition, as does engaging in strenuous exercise. Corticosteroids, drugs that dilate blood vessels, and certain blood pressure medications are known to make rosacea worse, mainly because they increase blood flow to the surface of the skin.
Reasons for choosing to have a rosacea treatment
Rosacea is not a dangerous condition, but because it affects the appearance, rosacea can cause psychological problems in those who are affected. If it remains untreated, the fallout from this condition may affect people’s social and work life as well.
Statistics from the U.S. show that although 78 percent of Americans did not know about rosacea, around 16 million are thought to be affected by it. According to the National Rosacea Society in the U.S., more than three quarters (76%) of patients said it had lowered their self-esteem and self-confidence. Around four in ten (41%) reported avoiding public contact or cancelling social engagements because of it. Among those suffering from severe rosacea symptoms, 88 percent reported that it had had an adverse impact on their professional interactions and over half (51%) reported having missed work because of it.
Left untreated, the condition becomes worse over time. Most people’s experience of rosacea is cyclic, with flare ups lasting weeks or months then going away slowly, only to reappear.
What to expect
Rosacea diagnosis is made clinically. In some cases a skin biopsy may be needed.
There is no known cure for rosacea. According to the National Rosacea Society (US), the keys to successfully managing rosacea include following prescribed long-term medical therapy, avoiding trigger factors and practicing appropriate skin care, including careful use of cosmetics. A combination of prescription medications and lifestyle changes can help control and manage rosacea symptoms. When medical therapy is given, it has to be tailored to each specific person.
Medical treatments for rosacea
Medical treatments for rosacea may mean combining prescription-strength topicals and oral medications. Applying prescribed topical medications such as a lotion, cream or gel to the skin once or twice a day will help reduce redness and inflammation.
According to the New Zealand Dermatological Society website DermNet, oral antibiotics like tetracycline help reduce the inflammation, redness, papules, pustules and the eye symptoms of rosacea. You will be asked to take the antibiotics for 6 to 12 weeks. The doses and duration will depend on the severity of rosacea. It may also be necessary to take an additional antibiotic course from time to time.
Ocular rosacea can be treated with either oral antibiotics or steroidal eye drops.
Most people notice an improvement in their rosacea within one or two months. If you stop taking the medications, the symptoms may return, which is why a long-term treatment is often necessary. Some changes that occur due to rosacea, such as the enlarging of blood vessels, redness and changes in the nose as with rhynophima, can become permanent.
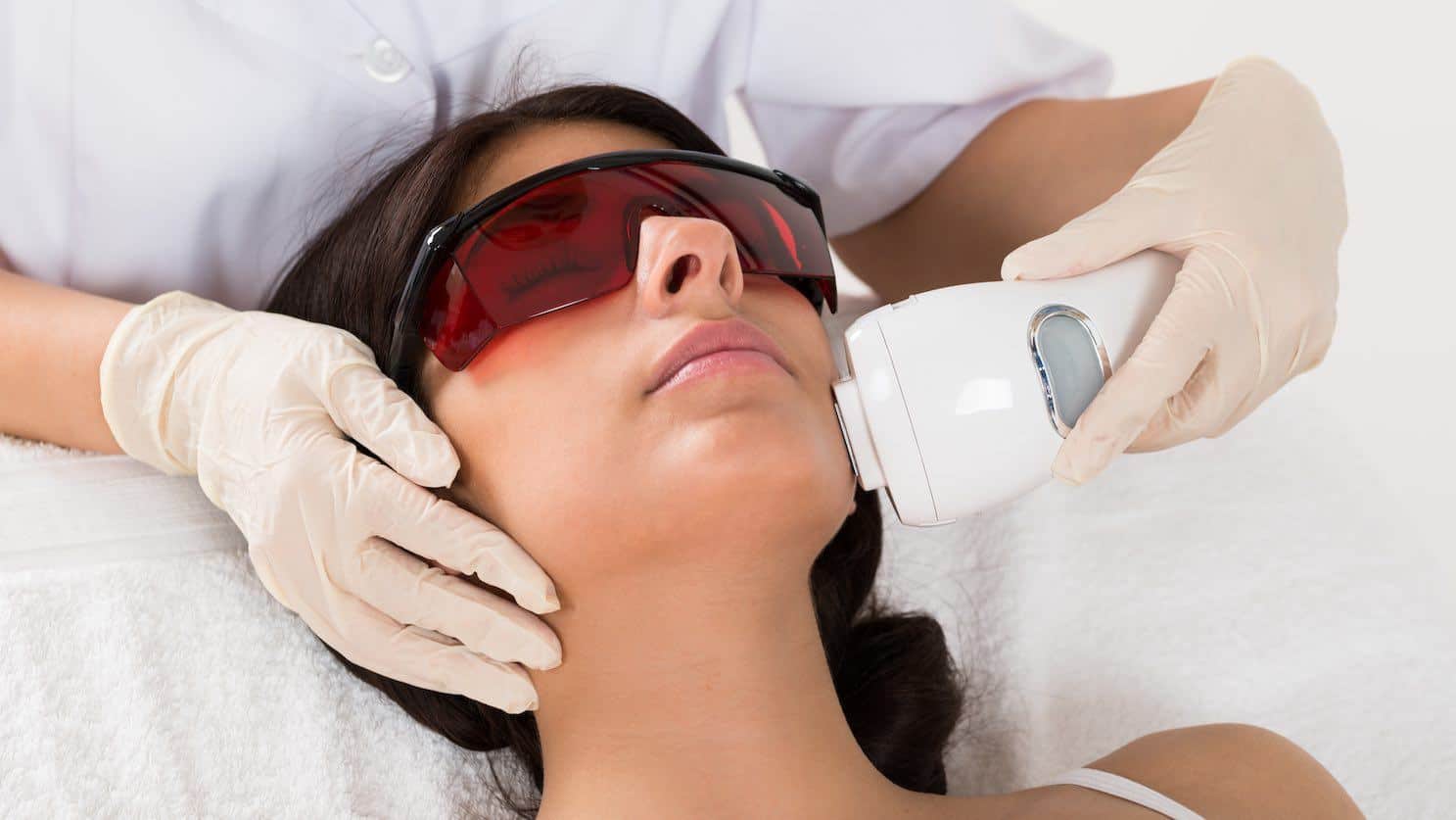
Surgical treatments, including laser surgery, can help reduce the visibility of blood vessels and improve the appearance overall. Red skin will respond well to laser and light treatments. Rosacea is known to respond well to intense pulsed light (IPL), vascular lasers, such as pulsed-dye laser, KTP lasers and Dornier 940nm lasers and carbon dioxide resurfacing. Fractional laser is usually not used for treating rosacea symptoms. Most laser treatments require a topical anaesthesia, but it is natural to experience some discomfort. There will be some bruising and swelling as well after IPL or pulsed-dye laser treatments.
You may need to take a couple of days off from work, but it is not essential. You can, if you wish, return to work the next day.
In the case of rhinophyma, surgery can also help remove and limit tissue build-up around the nose. A dermatologist can treat rhinophyma successfully by reshaping the nose surgically or with a carbon dioxide laser.
Lifestyle changes
Lifestyle changes you must make to keep rosacea in control include:
- Skin care – Certain moisturisers, mild cleansers and sunscreens will help improve the skin’s health. It is necessary to use water-based make-up and avoid oil-based facial creams.
- Protecting the skin from the sun – Choose light, oil-free sunscreens for your face.
- Menopause – If hot flushes that occur during menopause are triggering your rosacea, check with your doctor about medications to treat signs and symptoms of menopause.
- Keep away from topical steroids even though you may see a short-term improvement. After applying a topical steroid, you can typically expect rosacea to get worse over the next few weeks.
- Keep your face cool to reduce flushing. This means being extra careful with hot and spicy food and alcohol as well as minimising exposure to hot baths and showers and warm room temperatures.
Before and after a procedure
Most treatments for rosacea do not require special preparation. There are several things you can do to prepare for any surgery and these apply to surgeries for treating rosacea as well, including laser and IPL treatments.
There are general steps that can speed up the healing process after surgery. Follow these and your surgeon’s instructions carefully to ensure speedy healing and a good outcome.
A set of postoperative instructions will be given to you by your practitioner to help reduce the risk of complications during the recovery period. Make sure to follow those instructions to the word.
Possible risks and complications
Antibiotics
Long-term use of antibiotics can lead to bacterial resistance.
Oral antibiotics such as tetracycline, minocycline and erythromycin may result in stomach discomfort, diarrhoea and vomiting or nausea. They also cause a sore mouth or tongue in some people.
Any drug prescribed for severe cases of inflammatory rosacea may cause serious side effects, including bone or joint pain and depression. Rashes and skin infections are also likely to occur. For these reasons, people taking these medications must be closely monitored.
Laser and light treatments
As with any treatment, there are risks involved in each type of laser procedure that treats rosacea. You should be fully aware of the potential risks and complications involved in any procedure before you elect to go through with it. It is always better to err on the side of caution.
Just as you would discuss potential benefits before treatment, it is always advisable to ask your practitioner to address the potential risks as they apply to you. They can also advise you on how to avoid or minimise some types of risk.
Rough costs involved
The cost of treatment for rosacea depends on exactly what treatments will apply to you. They will vary according to the severity of your symptoms as well as the specific course of treatment your doctor or dermatologist recommends. Once your treatments have been recommended you will be given details about their costs.
Some Australian private health insurers may help pay for some of the rosacea treatments. You may also get Medicare rebates for some types of treatment for rosacea, including IPL treatments.
This information is correct as of 2019.
Additional information
- The Rosacea Support Group offers a lot of information on the condition and treatments from an Aussie perspective.
- The National Rosacea Society offers Rosacea Makeup tips and Skin Care and Cosmetic guidance on their website.
Hi
Have Laser surgery on my face for broken capillaries veins .
I was prescribed 7 days pill form of steroids . Is this extremely necessary to take during healing process for better results or is it just for a swelling purposes only. I am concerned of the side effects due to interfering with moods irritability weight gain agitation.
Hello Dr Davis. I am well overdue for some laser treatment of my nose and cheeks, and possibly also dysport. Would love to come in soon. No probs if I need to make multiple appointments.
PS – I am also keen to try this ultrasound skin shrinking of the face, cheeks and neck. As you know I can tolerate pain very well. Do you need models to train people on – eg me, or do you offer discounts for Nurses and / or no interest payment plans?